Living with Type 2 diabetes means you’re used to weighing risks before making health decisions. Dental care is no different. I speak with patients every week who assume diabetes automatically disqualifies them from dental implants. That assumption often keeps people living with missing teeth longer than necessary.
As a dental implant provider, my goal today is to give you straight answers—no exaggeration, no pressure, and no half-truths. With the right planning and medical coordination, many people with Type 2 diabetes can safely move forward with treatment. The key is understanding what matters, what doesn’t, and how preparation changes outcomes.
Let’s walk through it together.
How Type 2 Diabetes Affects Oral Healing
Type 2 diabetes impacts the body in ways that are especially relevant to implant dentistry. Elevated blood glucose levels can slow circulation, affect immune response, and reduce the body’s ability to heal after surgery. That doesn’t mean implants are off the table, but it does mean we have to approach treatment thoughtfully.
From a dental standpoint, the biggest concerns include:
- Delayed wound healing
- Higher risk of infection
- Increased likelihood of gum inflammation
- Changes in bone metabolism
Research published in the Journal of Clinical Periodontology shows that patients with well-controlled diabetes have implant success rates comparable to those without diabetes. Problems tend to arise when blood sugar remains poorly controlled over time.
That distinction matters more than the diagnosis itself.
Blood Sugar Control Matters More Than the Label
One of the first things I review isn’t whether someone has diabetes—it’s how well it’s managed. Hemoglobin A1C levels give us a reliable picture of blood sugar control over several months. Lower, stable A1C values are consistently associated with better surgical outcomes.
Patients who actively manage their diabetes through medication, nutrition, and routine medical care often heal predictably after implant placement. On the other hand, uncontrolled diabetes increases the chance of complications, regardless of age or overall health.
This is why collaboration with your primary care physician or endocrinologist is part of responsible implant planning.
Bone Health and Why It Deserves Special Attention
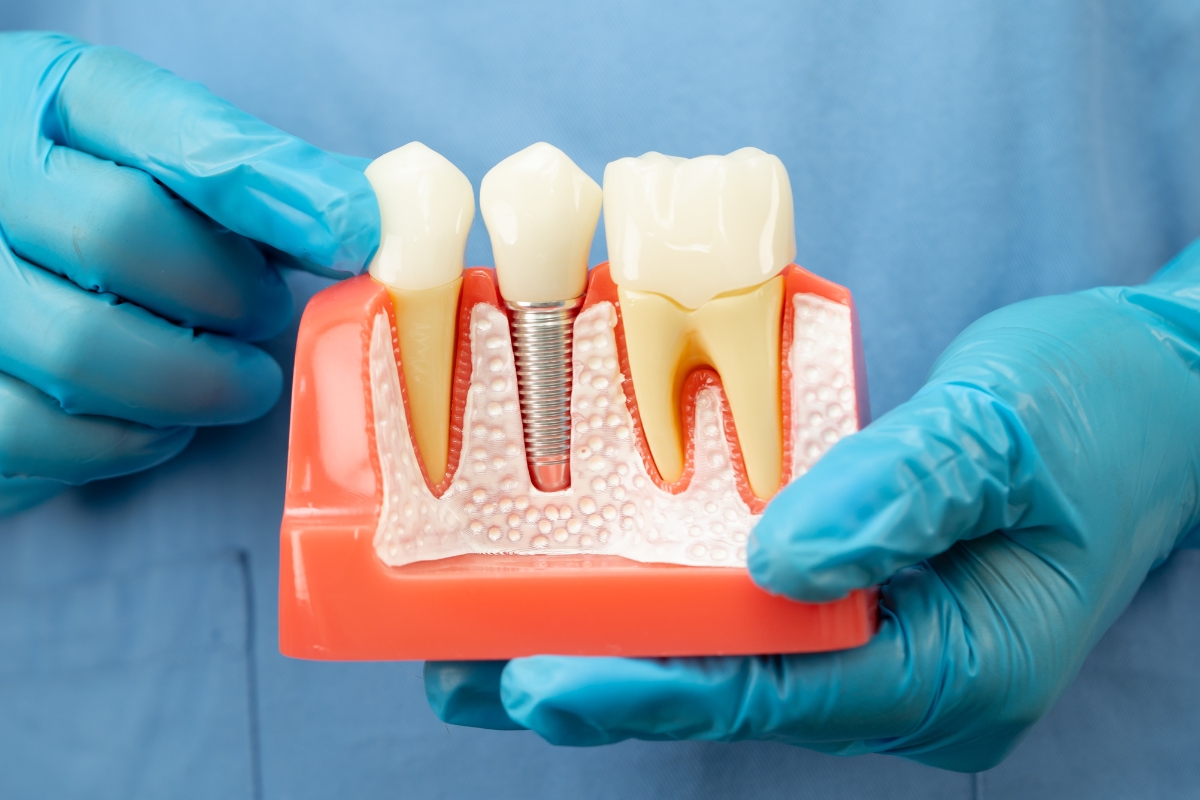
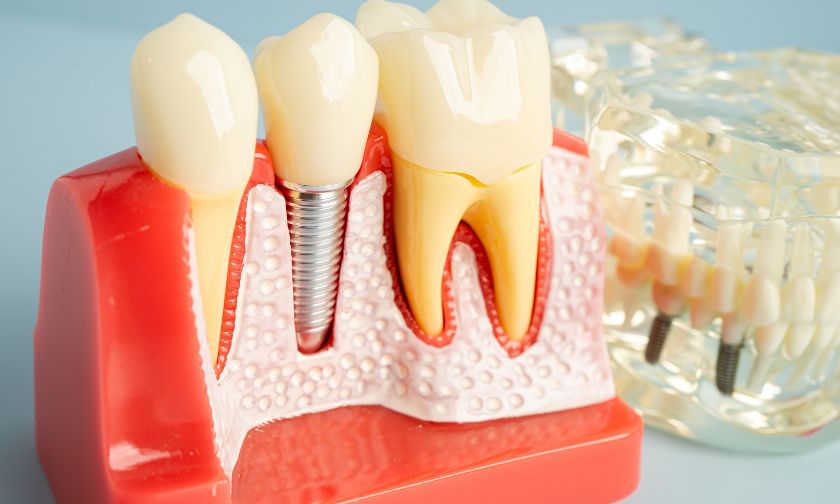
Dental implants rely on osseointegration, a biological process where bone grows around and anchors the implant. Diabetes can influence bone density and turnover, particularly in the jaw.
Before recommending treatment, I evaluate:
- Bone volume using advanced imaging
- Signs of active gum disease
- History of periodontal bone loss
- Areas of inflammation or infection
If bone support is limited, grafting may be discussed. Bone grafting in patients with controlled diabetes has shown favorable outcomes in multiple peer-reviewed studies, including data from the International Journal of Oral & Maxillofacial Implants.
The takeaway is simple: bone quality matters, but it can often be managed safely with proper planning.
Infection Risk and How We Reduce It
Diabetes can increase susceptibility to infection, which is why implant protocols must be precise. Preventive steps make a measurable difference.
These typically include:
- Treating gum disease before surgery
- Presurgical antibacterial rinses
- Conservative surgical techniques
- Clear post-operative care instructions
Good oral hygiene habits at home are equally important. Brushing, flossing, and routine professional cleanings directly influence long-term implant stability.
This is not about perfection. It’s about consistency.
Is Implant Failure More Common With Diabetes?
This question comes up often, and it deserves a clear answer.
Studies from organizations such as the American Academy of Implant Dentistry indicate that implant survival rates remain high in patients with controlled Type 2 diabetes. Failures are more strongly linked to smoking, untreated gum disease, and poor follow-up care than diabetes alone.
In other words, diabetes is a risk factor, not a disqualifier.
What the Evaluation Process Looks Like
For patients considering dental implants in Prairie Village, the evaluation process is thorough but straightforward. I start by listening—understanding your health history, concerns, and goals.
From there, we review:
- Medical history and medications
- Recent A1C values
- Jawbone imaging
- Gum health and bite alignment
This allows us to determine whether treatment can proceed immediately or if stabilization steps should happen first. Many patients appreciate having a clear roadmap rather than vague reassurance.
Timing Matters More Than Speed
Rushing implant treatment is rarely beneficial, especially for patients managing chronic conditions. Sometimes, waiting a few months to improve glycemic control leads to safer surgery and better long-term results.
This approach may not be flashy, but it’s grounded in evidence and patient safety.
What Improves Implant Success for Diabetic Patients
Before moving forward, I typically recommend focusing on:
- Stable blood sugar levels
- Healthy gums with no active infection
- Consistent oral hygiene routines
- Open communication between dental and medical providers
These factors influence outcomes more than age or diagnosis.
Type 2 diabetes does not automatically preclude dental implants. With careful evaluation, medical coordination, and realistic expectations, many patients achieve strong, lasting results.
If missing teeth are affecting how you eat, speak, or feel about your smile, it may be time for a conversation with us—not assumptions.
Schedule a consultation with Monarch Dental Care to discuss whether dental implants are right for you. A thoughtful plan today can prevent bigger oral health challenges down the road.
People Also Ask
Can dental implants affect blood sugar levels?
Implants themselves do not change blood sugar levels. However, untreated oral infections can contribute to systemic inflammation, which may influence glucose control. Addressing oral health can support overall wellness.
Should I take antibiotics before implant surgery?
Antibiotics are sometimes prescribed based on individual risk factors. This decision depends on medical history, current oral health, and surgical complexity.
How long does healing take with diabetes?
Healing timelines vary. Patients with stable blood sugar often heal within expected ranges, while uncontrolled diabetes can slow tissue repair.
Can implants fail years later because of diabetes?
Late implant failure is usually related to gum disease or lack of maintenance rather than diabetes alone. Regular dental visits play a major role in prevention.
Does diabetes change how implants feel?
Once healed, implants function like natural teeth. Diabetes does not alter sensation or comfort when integration is successful.rs. Gum can get stuck to your aligners, affecting the fit and movement of your teeth.